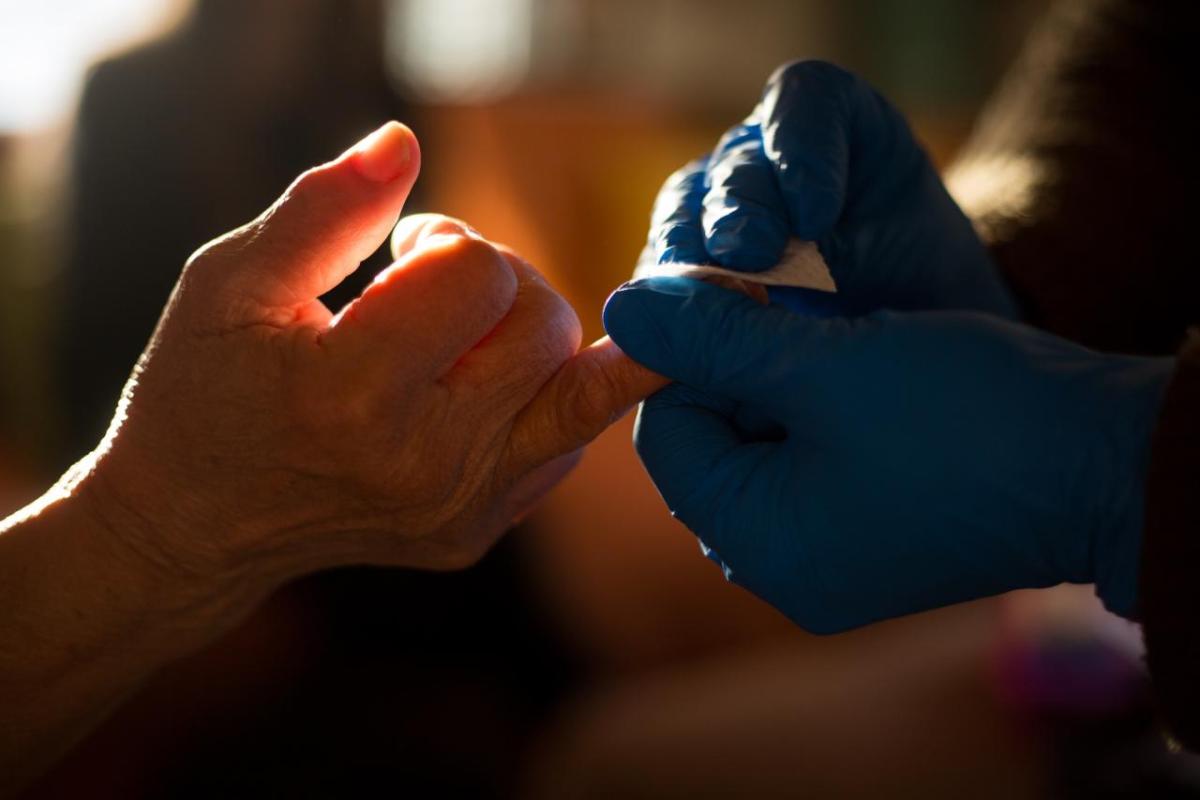
A community-based healthcare system in Camden, New Jersey, is improving patients’ health by considering every aspect of their life a part of the treatment.
Originally published on TriplePundit.
Amy Brown February 27, 2026
It’s not often that landing in the hospital is a stroke of good luck. For Charmaine, who faced multiple health issues and the recent loss of two sons, it was a godsend. It was there that the Camden, New Jersey, resident learned she qualified for a community-based healthcare system called the Healthy Neighbor program.
The hospital contacted the Healthy Neighbor team, and soon, Charmaine was sitting in her home with community health worker Fanny Ochoa instead. As they chatted, Ochoa determined that Charmaine needed help to manage her type 2 diabetes and chronic obstructive pulmonary disease (COPD). That also meant finding an affordable housing solution, and taking care of her mental and emotional health amidst overwhelming grief after the loss of her sons.
Ochoa told Charmaine that she would support her over the next year to improve all aspects of her health and well-being. Now, they were a team.
“She was just everything that I needed at the time,” Charmaine told TriplePundit. “My sugar is under control, and my COPD is not an issue. And I live in a beautiful new apartment, thanks to the program.”
Healthcare beyond the doctor’s office
The Healthy Neighbor program, led by healthcare provider Virtua Health and supported by global medical technology company Medtronic and Medtronic LABS, recognizes that health goes beyond medicine and visits to the doctor. A person’s wellbeing is just as much shaped by where they live, their opportunities and their challenges.
The aim is to build the kind of trust that tackles both the clinical and social determinants of health by pairing community health workers directly with patients over a long period of time. The program targets adults with type 2 diabetes or hypertension, providing up to one year of monthly home visits to identify and address barriers to their health.
Charmaine’s story reflects a larger crisis in Camden. In the city of 70,000, residents live up to 16 years less than people just 6 miles away. Many of the significant, long-standing health disparities are driven by poverty and environmental factors. By bringing technology and trust directly to people’s homes, the program addresses root causes of poor health, and it’s working.
Ochoa was able to support Charmaine in a more sustainable way by considering every aspect of her life as a part of her treatment. To help manage her diabetes, Ochoa provided Charmaine with a tiny wearable sensor that provides real-time, continuous glucose monitoring. She also encouraged her to apply to live at Oliver Station, an affordable housing solution with on-site primary care in Camden developed by the Michaels Organization and Virtua Health.
“I am so grateful to [Ochoa] and the program. If it wasn’t for her, I wouldn’t be here,” Charmaine said. “She’s been with me every step of the way. My new home is beautiful. I just thank God for this program because they have helped me so much.”
La Shawn Dutton-Spruill, a community health worker with Healthy Neighbor, can recount similar success stories. Dutton-Spruill met her patient Denise while she was living in a condemned building with uncontrolled hypertension and type 2 diabetes. Denise was missing doctor’s appointments, skipping medications and falling through the cracks of the system.
In the initial assessment, she checked Denise’s basic health vitals but also discussed other aspects of her situation, including housing and access to healthy food. Together, they came up with goals. Every two weeks, Dutton-Spruill checked in.
Healthy food access is very important for people with a food-impacted chronic condition like diabetes, Dutton-Spruill said. If patients are struggling to access it, Healthy Neighbor connects them with Virtua Health’s Eat Well program, which delivers fresh fruits and vegetables to underserved areas. They can purchase items with “food bucks” provided by the program, their federal Supplemental Nutrition Assistance Program (SNAP) benefits or a debit card.
Today, Denise is living in safe housing, manages her prescriptions, and is stabilizing her hypertension and type 2 diabetes.
“She’s just a totally different person. The program turned her all the way around,” Dutton-Spruill said. “She was suffering from depression, and now, she’s going out on the weekends. She’s very happy, meeting the program’s expectations and living her life to the fullest.”
Denise and Charmaine are part of the 74 percent of patients with uncontrolled hypertension who saw a meaningful improvement in blood pressure control after participating in Healthy Neighbor. Just under 70 percent of type 2 diabetic patients in the program saw a drop in blood sugar levels, too.
A model others can copy
Healthy Neighbor can’t solve such a complex set of problems entirely on its own, so it partners with local organizations like nonprofits, food banks and other clinical organizations.
“If a patient is currently experiencing homelessness, before we can even talk about reducing their blood sugar levels or hypertension, we need to figure out how to get them to a better and more reliable housing situation,” said Daniel Master, director of community health and impact at Virtua Health. “Our team has done a great job of connecting numerous patients to housing options within the city, and then, we see measurable clinical improvements that follow from there.”
Learning about the wide range of support locally available to them can be life-changing for the people the program serves, Master said. “These are patients who traditionally have not had as much access to or understanding of the larger health systems as patients from other communities.”
The goal is a long-term solution to people’s ongoing health that they can uphold themselves after the year-long program ends. “We bring all of those resources to patients so that their care can be sustainable,” Master said. “We know that our intervention is up to 12 months, and a lot is going to happen after that year.”
The program is expanding locally thanks to a grant from the city of Camden to grow the community health worker team and reach more patients. And Virtua Health and Medtronic LABS released a toolkit to help hospitals nationwide to replicate the model. Meanwhile, plans to expand the program beyond Camden are also in the works.
“Our hypothesis for why we are so successful is because we are addressing the social and clinical factors of health in one model and leveraging the resources of a large health system,” Master said. “We want to open source it because we know what we’re doing is unique.”
One thing standing in the way of that growth is the lack of a reliable reimbursement mechanism to fund the services of community health workers in the same way that nutrition and education services are funded by insurers, Master said.
Limited awareness that a model like this is an option is another. “Community health workers have been deployed in many health systems and in many environments. But not, we believe, in the way that we’re deploying them,” Master said. “In terms of sustainability that is the key.”
Housing, financial challenges and health food access will continue to be a perennial issue for communities, Master said. “There’s still a lot more that could be done by having healthcare work with the government and social service sector. We believe we are paving the way for what that could look like,” he added. “We know that this is an intervention that works.”
Editor’s Note: Program participants are referred to by their first name to protect patient privacy. This story was updated on March 3, 2026.